Microsurgical Vasectomy Reversal
Robert U. Finnerty M.D. FACS
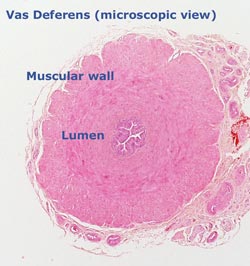
Vasectomy is a minor surgical procedure for permanent male fertility control, performed on about 700,000 men each year in the United States. The duct which carries sperm from the testicle (called the vas deferens) is cut and sealed in order to prevent sperm from leaving the testes. The vas deferens measures about 1/10th of an inch in diameter (2.5 mm), the majority of which is a thick muscular wall. The actual passageway for the sperm (called the lumen) measures less than 1/100th of an inch (0.25 mm).
The testes continues to produce sperm after a vasectomy — this is what makes vasectomy reversal possible. The challenge is to accurately reconstruct the duct system, which is extremely small and delicate. While the vas is very easy to cut, it is much more difficult to successfully reconnect. After vasectomy, there is continued production of a small amount of sperm fluid from the testes. This results in a slight increase in pressure in the vas below the site of the vasectomy, which over time will stretch the inside of the vas duct. As a result, the inside diameter of the vas below the vasectomy site is often 3-5 times larger than the original diameter above the vasectomy.
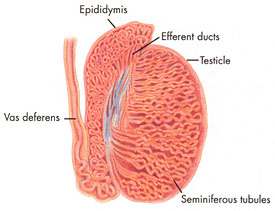 As the vas deferens gets closer to the testes (below the vasectomy site), its thick muscular wall thins out and disappears, and it merges into a structure called the epididymis. This portion of the duct is attached to the testes, and it contains nearly 20 feet of a delicate, coiled microscopic tubule. Back pressure from ongoing sperm production and the blockage caused by vasectomy may cause this delicate tubule to become extremely thin and rupture over time (this is sometimes called a “blowout“).
As the vas deferens gets closer to the testes (below the vasectomy site), its thick muscular wall thins out and disappears, and it merges into a structure called the epididymis. This portion of the duct is attached to the testes, and it contains nearly 20 feet of a delicate, coiled microscopic tubule. Back pressure from ongoing sperm production and the blockage caused by vasectomy may cause this delicate tubule to become extremely thin and rupture over time (this is sometimes called a “blowout“).
When this occurs, the resulting inflammation will cause scarring and a secondary blockage, (which may be partial or complete) between the testes and the vasectomy site. Even precise repair of the vasectomy site, without addressing this epididymal obstruction, will result in failure to restore fertility.
The problem of epididymal obstruction becomes more likely as the time after vasectomy increases — although it is quite common even in men only a few years out. While most men have few problems after vasectomy, a small percentage may also experience post-vasectomy pain, either intermittently with sexual activity, or in some instances, on a chronic basis. When this occurs, it can be a difficult and frustrating problem to overcome, as medical therapy rarely if ever helps. Surgery to reverse the vasectomy is almost always the best solution to this challenging complication of vasectomy.